My breast reconstruction patients benefit tremendously even after the operation. The BairHugger is kept on overnight- it keeps the 'breast flap' warm and hence keeps the connected blood vessels which are 2-3mm in diameter flowing nicely. My reconstruction patients do feel a little 'roasted', though I prefer to say 'cosy'!.
|
Invented in 1987, forced-air warming technology, the Bair Hugger™shown in the photo, looks like a plastic blanket with warm air inside, has become standard in hospitals around the world, safely warming 165+ million patients. It keeps anaesthetised patients warm and maintains 'normothermia' - normal body temperature. This makes the operation safer for the patient and as it is single-use, reduces infection. Maintaining normal body temperature is crucial in long operations, especially breast reconstructions which I do every week; when a large part of the body such as the chest and abdomen are exposed for surgery, thereby losing heat and cooling down further from the use of damp swabs and saline in the surgical field.
My breast reconstruction patients benefit tremendously even after the operation. The BairHugger is kept on overnight- it keeps the 'breast flap' warm and hence keeps the connected blood vessels which are 2-3mm in diameter flowing nicely. My reconstruction patients do feel a little 'roasted', though I prefer to say 'cosy'!.
0 Comments
Background. Single mastectomy and full axial clearance September 2011. Six chemo cycles, Herceptin radiotherapy followed by Anastrazole beginning in April 2012. At Anita’s suggestion, I’m pleased to provide this text as a possible help for anyone who’s thinking of having breast reconstruction and/or maybe their family/friends.
Why did I choose reconstruction? · Practicality: wear more of my clothes ; not flashing a prosthesis or the sunken chest · To reclaim something back from cancer; I want my body back · Because I can. Isn’t a lot to go through – just for a new breast? Maybe. My view is that these weeks/months are only a snapshot amongst hopefully many more years of life to experience with greater confidence. What did my partner, family, friends etc think about reconstruction? In short, everyone was supportive, expressing only concern for my wellbeing. Close family were reassured by my/partners confidence in the surgical and nursing teams. There were a few “interesting” comments from acquaintances – based on (some) understandable ignorance- about my motive, the procedure and the outcome. Free cosmetic surgery it is not. Was there a time, pre-op, when you wondered if you were doing the right thing for you? September 2013, Tuscany, 30 degrees Centigrade. I’m floating in a clean, quiet swimming pool, staring up at azure sky. Screeches of high soaring kites cut through the purlopp,plop.lurrop as the cool water laps my ears. Occasional breezes rustle through the surrounding cypress trees. Yesterday’s sightseeing is rewarded with today’s lazy, lazy, warm, warm relaxing mmmm. Nearly 12 months of rigorous exercise has produced a body which I’m not entirely ashamed - and wearing a bikini – with a well disguised prosthesis. I’m jolly well going to enjoy milestone: my first proper holiday abroad – since I finished all my hospital treatment. Suddenly, an exuberant party of Italians arrives . “Careful”, my partner says: the prosthesis has come loose and I push it back into the pocket. We maintain prosthesis vigilance although I’m self-conscious about my necessary, frequent checking. But the decision to reconstruct is made and a surgery date pencilled in – wonderful – I can look forward to not worrying about a prosthesis embarrassing me in public. This was when I knew I was making the right decision for me. It was SOOOO the right decision. Day before op Quite calm. Uneventful journey to East Grinstead. Partner staying more locally and he’ll return to me early next morning before I journey to theatre. Relaxing evening with hot chocolate – and then sleep. That morning. At 06.30, I’m woken up for the cup of black tea, which the anaesthetist has insisted I should drink to give my stomach something to work on. My family would know this is no hardship (I’m a tea pot) and I’m very pleased to have it. From previous experience, I know these next two hours before going to theatre will pass quickly in a series of visits from various medics. Oh! That trolley man arrived quickly – they always do! Usual pre-general anaesthetic prep and chat covers the usual “gin and tonic” joke from the anaesthetist, moves on to brief shared appreciation for Tuscany - and then I tell them how far the “gin and tonic” is reaching….. Much later that same day: back in my (dark) room. Very very thirsty Sooooo.so tired. The night passes with frequent obs, sips of water, presumably some sleep and it’s so flipping HOT and STUFFY: heat that helps the relocated blood vessels in the new flap (breast) to “flow”. Day One post-op. Still very hot. Partner visited for several hours – but I can’t remember much. Day Two post-op Nurses and Anita are very happy with the way the flap is taking. I tackle a trip to the bathroom , and with the help of a nurse, walk around the room and out and up the corridor . Chuffed – up and about! Day Three One or two drains were removed today which makes things a bit more comfortable. Day Four Is shower day. Anita’s daily check confirms healing progressed sufficiently to permit a shower with assistance – hurrah I feel and smell soooooo much better - fresssssssshhhhhhhh. A nurse tactfully agrees I smell better. Day Five Nurses introduce me to a lovely woman up the corridor who’s a couple of days ahead of me in her DIEP with a different surgeon. We compare pants, support bras and post-chemo haircuts. I’m always pleasantly surprised how good it is to share our experiences: always positive, encouraging, uplifting, funny, reassuring, enlightening, educative. One week post op A bit uncomfortable – but hey - I don’t regret this whatsoever. Two weeks post op and at home Unexpectedly, I’m having difficulty remembering what my pre-op left side looked like – and I like this very positive surprise and acceptance of my new form. Prosthesis - I do not need it any more. I do not need it any more. Haha About three weeks post surgery Recuperating at home. In bed, snug and warm and a cat for company. My fellow DIEP-er emails to confirm she’s recovering well, with the support of family and friends. Christmas is a-coming!! What does your partner think of the work? After reassuring him the sight was not gruesome, he did look and pronounced the new breast as “very good”. Four weeks post surgery/what continues to surprise you? I still relish the comparatively novel experience of putting on bra with all me in it. Haha. That my 54 year old body healed so quickly, but I must respect it: no heavy lifting, no cycling, definitely no power plate exercising or horse riding for about 12 weeks ( I think). Subsequent follow up with Anita confirms all scars healing very – and joy - I no longer have to wear a bra or the big pants at night . Eight weeks at home Pre Xmas drinks at friends. New tight trousers and loving my new bonus flat tummy. Later at home, I realise that at no point did I even consider the location and look of a left breast. There was no hoiking back a prosthesis into position, no fidgeting. I think to myself, this is what it used to be like – just getting on and being and doing, without e.g. a prosthesis reminding me of its existence and hence (sorry to say) of cancer. That’s a positive I hadn’t anticipated – in that way - nor so soon. Four months post surgery Next follow-up today with Anita. As anticipated, there may be some re-alignment required if I choose to – but, you know what - I’d be happy with what I’ve got if I didn’t go down that route as I’m already a new woman! The result is fantastic and I’m so grateful to Anita and her team for their expertise, skill and care. Let’s see what today brings!! 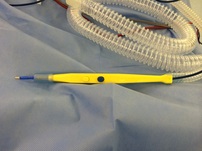 The picture on the left shows the new generation diathermy machines used today, and is one I always use during most operations. Electrosurgical units (diathermy machines) were first introduced during the early twentieth century to facilitate stopping bleeding by closing off the ends of cut blood vessel ends (haemostasis) and/or the cutting of tissue during surgical procedures. In this process, a smoke plume is generated which is sucked up by the attached smoke evacuation tubing. It has revolutionised the way I operate. Bleeding during surgery is kept to a minimum. Infact, it is rare for my patients to require blood transfusion even after major reconstruction surgery lasting 6-7 hours. The incidence for returning to theatre for an emergency evacuation of a haematoma (removing blood clot in the tissues) has decreased significantly, compared to the days when one used to use a knife throughout the operation. The downside of using a diathermy to perform the operation is the generation of heat in the tissues, which can cause thermal damage. To reduce this risk, I will often use it on low settings of 'pure' current- so that even if the diathermy tip accidentally touches my gloved finger, there is minimal heat and no burn. As a result of reducing bleeding during operations, the diathermy has made my dissections cleaner and faster, as the operating field is clear. Patients have benefitted too- less blood loss and reduced operation times means a quicker recovery after major surgery.  To make a breast with skin and fat from the tummy or inner thigh after a mastectomy, involves some 'plumbing'. The tummy or inner thigh tissue with its blood supply is completely disconnected and detached from the body. It is then placed on the chest and the blood vessels or 'pipes' are connected to those under the ribs. The size of the these 'pipes' is very small- between 1 to 3 mm in diameter. So similar to a plumbing pipe-coupler, plastic surgeons use a coupling device as shown in the picture, to join up the vein using an operating microscope. This has reduced the time taken to connect the veins from 45-50 mins when sutured by hand, down to approximately 8 mins when the coupler is used. In an operation that takes 6 hours , this is a significant time saving and results in less time under an anaesthetic for the patient. And it ensures that a sidewall of the vein is not caught up in a stitch, something one has to look out for in a hand-sewn 'plumbing' of the vein. For the last 8 years, every Tuesday, when I reconstruct a breast using skin and fat from the tummy (DIEP) or from the inner thigh (TUG), I count the venous coupler as one of my blessings- it makes my surgical life a little bit safer, quicker and more controlled, both for me and for my patients. 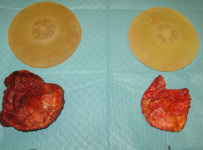 This photo shows the thick capsule (scar tissue) that has been removed from around old intact implants. Grade IV capsule contracture is when the breast becomes hard, painful and distorted. Prevention is the key, however, as we do not the causes of capsular contracture, this is aimed at good surgical technique, including the use of a mixture of antibiotic solutions to irrigate the breast cavity before placement of implant. This can reduce the capsular contracture rate from 12% to 2%. However, when it does occur, treatment is usually surgical, in the form of capsulectomy (total removal of the capsule). There has been limited success with the use of the asthma drug Accolate in softening the capsule in 50%. To read more, go to the procedure page on Breast implants which tells you everything you need to know about breast implants. 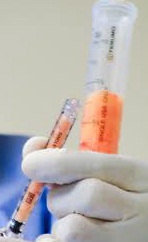 Fat transfer in breasts has been in the news over the last year. It involves removing fat in an atraumatic way from parts of the body such as hips, abdomen and thighs and re-injecting it into the breast either to enhance its volume usually by a cup size for breast augmentation or to fill small defects after breast cancer lumpectomy surgery. Great care has to be taken to transfer fat into the subcutaneous or intrapectoral planes and not to inject fat into the breast tissue itself. As the fat can re-absorb by 30- 40%, two or more ‘top-up ’operations may be required. On MRI or mammograms, the resorption can be seen as calcification. A trained radiologist can distinguish between microcalcification arising from fat transfer vs. breast cancer. However, there is limited scientific evidence regarding the effect of stem cells, contained within the transferred fat, on breast cancer. Studies in the laboratory have shown that presence of stem cells favour the growth of tumour cells, but this has not yet been substantiated by clinical trials. The American Society of Plastic Surgeons (ASPS) has advised mammograms before and after fat transfer to provide re-assurance to the patient regarding any new abnormalities that may develop. It advises against fat transfer in cosmetic patients at high-risk of breast cancer such as those with personal or familial history of breast cancer and/or BRCA-1, BRCA-2 gene inheritance. In the UK, guidelines from the Breast Interface group (BAPRAS and BASO) were published in 2012 are available on the link: http://www.bapras.org.uk/downloaddoc.asp?id=666.  After any breast surgery, the supporting ligaments in the breasts are put under strain or have been divided either partially or completely. When you have Breast Implants or Breast Uplift/ Reduction surgery, the breast gland is lifted off the underlying muscles too. Hence, for 12 weeks afterwards it is important to avoid any bouncing movements such as running, trampolining, body pump, aerobics, circuit training or horse-riding. After this period, it is crucial to wear a good sports bra during sporing activities to maintain the surgical results that have been achieved. A Running Level sports bra such as the Shockabsorber will reduce bounce by as much as 60-75%. Wearing a lycra crop top above this will reduce the breast movement even more by providing compression.  I almost always use tan coloured micropore tape for surgical sites as a dressing both for my cosmetic and reconstructive surgery patients. Once the first dressing change has been done, you will be advised to re-apply the micropore tape without tension to support the scar for 3-4 weeks after surgery. In the first 2 weeks, the tape can be left on. However, after showering (no baths!), dab the tape dry with paper towel and then using a hair-dryer on a cold setting, blow dry the tape until 'bone-dry'. Do not leave it damp as this can make the underlying wound/ scar soggy. The tape is latex-free, hypoallergenic and kind to fragile skin. It is microporous, which means it is not occlusive and hence the need to ensure the tape is dry after showering! When changing the tape, start off at one end and peel off, low and slow back over itself, supporting the fragile skin underneath with your fingers. There is anecdotal evidence of surgical wound cross infection from household pets. Ensure you have clean bedsheets when you return home after surgery and do not allow pets in your bedroom and no cuddles for the first 3-4 weeks! Once you have stopped using the tape 4 weeks after surgery, massage the scar with pressure using a non-perfumed cream or bio-oil (do not use an old pot or bottle incase it is harbouring bugs, buy a new one!) for several weeks to months, and always use high sun-block for the first year in the sun. Remember scars do take a year or so to fade. |
Archives
February 2020
Categories
All
|



 RSS Feed
RSS Feed





