| so_tunbridge_wells_the_great_round_table_debate_.pdf |
|
0 Comments
Invented in 1987, forced-air warming technology, the Bair Hugger™shown in the photo, looks like a plastic blanket with warm air inside, has become standard in hospitals around the world, safely warming 165+ million patients. It keeps anaesthetised patients warm and maintains 'normothermia' - normal body temperature. This makes the operation safer for the patient and as it is single-use, reduces infection. Maintaining normal body temperature is crucial in long operations, especially breast reconstructions which I do every week; when a large part of the body such as the chest and abdomen are exposed for surgery, thereby losing heat and cooling down further from the use of damp swabs and saline in the surgical field.
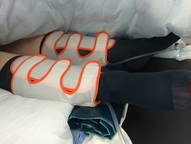
My breast reconstruction patients benefit tremendously even after the operation. The BairHugger is kept on overnight- it keeps the 'breast flap' warm and hence keeps the connected blood vessels which are 2-3mm in diameter flowing nicely. My reconstruction patients do feel a little 'roasted', though I prefer to say 'cosy'!. Flowtron Boots are absolutely vital during lengthy operations. The photo on the left shows a patient with dark TED stockings on (like flight stockings to prevent blood clots in legs) and white flowtron boots applied over the TEDs. Flowtrons are connected to a pump with flexible tubes. The pump inflates the Flowtrons intermittently and stimulates the flow of blood through the deep veins, pushing blood back towards the heart. It then deflates. This action copies how veins are squeezed by muscles when you walk.
Flowtrons boots prevent deep vein thrombosis (blood clots in legs) during surgery. Along with TED surgical stockings, they are an every-day surgical device we take for granted. TED surgical stockings and Flowtron boots are used in almost all the operations I perform every week. Another of my unsung surgical heroes that have made surgery safer for patients today. Background. Single mastectomy and full axial clearance September 2011. Six chemo cycles, Herceptin radiotherapy followed by Anastrazole beginning in April 2012. At Anita’s suggestion, I’m pleased to provide this text as a possible help for anyone who’s thinking of having breast reconstruction and/or maybe their family/friends.
Why did I choose reconstruction? · Practicality: wear more of my clothes ; not flashing a prosthesis or the sunken chest · To reclaim something back from cancer; I want my body back · Because I can. Isn’t a lot to go through – just for a new breast? Maybe. My view is that these weeks/months are only a snapshot amongst hopefully many more years of life to experience with greater confidence. What did my partner, family, friends etc think about reconstruction? In short, everyone was supportive, expressing only concern for my wellbeing. Close family were reassured by my/partners confidence in the surgical and nursing teams. There were a few “interesting” comments from acquaintances – based on (some) understandable ignorance- about my motive, the procedure and the outcome. Free cosmetic surgery it is not. Was there a time, pre-op, when you wondered if you were doing the right thing for you? September 2013, Tuscany, 30 degrees Centigrade. I’m floating in a clean, quiet swimming pool, staring up at azure sky. Screeches of high soaring kites cut through the purlopp,plop.lurrop as the cool water laps my ears. Occasional breezes rustle through the surrounding cypress trees. Yesterday’s sightseeing is rewarded with today’s lazy, lazy, warm, warm relaxing mmmm. Nearly 12 months of rigorous exercise has produced a body which I’m not entirely ashamed - and wearing a bikini – with a well disguised prosthesis. I’m jolly well going to enjoy milestone: my first proper holiday abroad – since I finished all my hospital treatment. Suddenly, an exuberant party of Italians arrives . “Careful”, my partner says: the prosthesis has come loose and I push it back into the pocket. We maintain prosthesis vigilance although I’m self-conscious about my necessary, frequent checking. But the decision to reconstruct is made and a surgery date pencilled in – wonderful – I can look forward to not worrying about a prosthesis embarrassing me in public. This was when I knew I was making the right decision for me. It was SOOOO the right decision. Day before op Quite calm. Uneventful journey to East Grinstead. Partner staying more locally and he’ll return to me early next morning before I journey to theatre. Relaxing evening with hot chocolate – and then sleep. That morning. At 06.30, I’m woken up for the cup of black tea, which the anaesthetist has insisted I should drink to give my stomach something to work on. My family would know this is no hardship (I’m a tea pot) and I’m very pleased to have it. From previous experience, I know these next two hours before going to theatre will pass quickly in a series of visits from various medics. Oh! That trolley man arrived quickly – they always do! Usual pre-general anaesthetic prep and chat covers the usual “gin and tonic” joke from the anaesthetist, moves on to brief shared appreciation for Tuscany - and then I tell them how far the “gin and tonic” is reaching….. Much later that same day: back in my (dark) room. Very very thirsty Sooooo.so tired. The night passes with frequent obs, sips of water, presumably some sleep and it’s so flipping HOT and STUFFY: heat that helps the relocated blood vessels in the new flap (breast) to “flow”. Day One post-op. Still very hot. Partner visited for several hours – but I can’t remember much. Day Two post-op Nurses and Anita are very happy with the way the flap is taking. I tackle a trip to the bathroom , and with the help of a nurse, walk around the room and out and up the corridor . Chuffed – up and about! Day Three One or two drains were removed today which makes things a bit more comfortable. Day Four Is shower day. Anita’s daily check confirms healing progressed sufficiently to permit a shower with assistance – hurrah I feel and smell soooooo much better - fresssssssshhhhhhhh. A nurse tactfully agrees I smell better. Day Five Nurses introduce me to a lovely woman up the corridor who’s a couple of days ahead of me in her DIEP with a different surgeon. We compare pants, support bras and post-chemo haircuts. I’m always pleasantly surprised how good it is to share our experiences: always positive, encouraging, uplifting, funny, reassuring, enlightening, educative. One week post op A bit uncomfortable – but hey - I don’t regret this whatsoever. Two weeks post op and at home Unexpectedly, I’m having difficulty remembering what my pre-op left side looked like – and I like this very positive surprise and acceptance of my new form. Prosthesis - I do not need it any more. I do not need it any more. Haha About three weeks post surgery Recuperating at home. In bed, snug and warm and a cat for company. My fellow DIEP-er emails to confirm she’s recovering well, with the support of family and friends. Christmas is a-coming!! What does your partner think of the work? After reassuring him the sight was not gruesome, he did look and pronounced the new breast as “very good”. Four weeks post surgery/what continues to surprise you? I still relish the comparatively novel experience of putting on bra with all me in it. Haha. That my 54 year old body healed so quickly, but I must respect it: no heavy lifting, no cycling, definitely no power plate exercising or horse riding for about 12 weeks ( I think). Subsequent follow up with Anita confirms all scars healing very – and joy - I no longer have to wear a bra or the big pants at night . Eight weeks at home Pre Xmas drinks at friends. New tight trousers and loving my new bonus flat tummy. Later at home, I realise that at no point did I even consider the location and look of a left breast. There was no hoiking back a prosthesis into position, no fidgeting. I think to myself, this is what it used to be like – just getting on and being and doing, without e.g. a prosthesis reminding me of its existence and hence (sorry to say) of cancer. That’s a positive I hadn’t anticipated – in that way - nor so soon. Four months post surgery Next follow-up today with Anita. As anticipated, there may be some re-alignment required if I choose to – but, you know what - I’d be happy with what I’ve got if I didn’t go down that route as I’m already a new woman! The result is fantastic and I’m so grateful to Anita and her team for their expertise, skill and care. Let’s see what today brings!! 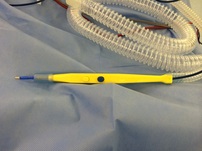 The picture on the left shows the new generation diathermy machines used today, and is one I always use during most operations. Electrosurgical units (diathermy machines) were first introduced during the early twentieth century to facilitate stopping bleeding by closing off the ends of cut blood vessel ends (haemostasis) and/or the cutting of tissue during surgical procedures. In this process, a smoke plume is generated which is sucked up by the attached smoke evacuation tubing. It has revolutionised the way I operate. Bleeding during surgery is kept to a minimum. Infact, it is rare for my patients to require blood transfusion even after major reconstruction surgery lasting 6-7 hours. The incidence for returning to theatre for an emergency evacuation of a haematoma (removing blood clot in the tissues) has decreased significantly, compared to the days when one used to use a knife throughout the operation. The downside of using a diathermy to perform the operation is the generation of heat in the tissues, which can cause thermal damage. To reduce this risk, I will often use it on low settings of 'pure' current- so that even if the diathermy tip accidentally touches my gloved finger, there is minimal heat and no burn. As a result of reducing bleeding during operations, the diathermy has made my dissections cleaner and faster, as the operating field is clear. Patients have benefitted too- less blood loss and reduced operation times means a quicker recovery after major surgery.  To make a breast with skin and fat from the tummy or inner thigh after a mastectomy, involves some 'plumbing'. The tummy or inner thigh tissue with its blood supply is completely disconnected and detached from the body. It is then placed on the chest and the blood vessels or 'pipes' are connected to those under the ribs. The size of the these 'pipes' is very small- between 1 to 3 mm in diameter. So similar to a plumbing pipe-coupler, plastic surgeons use a coupling device as shown in the picture, to join up the vein using an operating microscope. This has reduced the time taken to connect the veins from 45-50 mins when sutured by hand, down to approximately 8 mins when the coupler is used. In an operation that takes 6 hours , this is a significant time saving and results in less time under an anaesthetic for the patient. And it ensures that a sidewall of the vein is not caught up in a stitch, something one has to look out for in a hand-sewn 'plumbing' of the vein. For the last 8 years, every Tuesday, when I reconstruct a breast using skin and fat from the tummy (DIEP) or from the inner thigh (TUG), I count the venous coupler as one of my blessings- it makes my surgical life a little bit safer, quicker and more controlled, both for me and for my patients.  At my NHS hospital, it is one of my duties as a Consultant to teach and mentor trainee plastic surgeons. A recent trainee feedback survey on the Consultants as trainers, showed that though I scored better than average in my 'trainer' skills, there were improvements that I could undertake in my teaching style, as demonstrated by the comments below:
Though I am not Shrek or an Ogre at work, I obviously do need to improve! Sometimes I must appear to be unapproachable, even though I feel I am not. And I have often wondered if, perhaps, the direct manner in which I speak gives rise to this perception. My second sin is that, I will form an opinion about a trainee in the first 2 weeks or so. If I find the trainee surgeon unreceptive, arrogant, lazy or rude to staff /patients, I do not give him/her the same support I would have otherwise. As a teacher, irrespective of trainee attitudes , I should be encouraging to all. And that is the difficult part.  Approaching 40, juggling home and work, was making me feel that I needed more than 24 hrs in a day. I was flat out, managing a busy breast reconstruction & aesthetic practise, and needed to keep running just to stay still. I was often taking my troubles home and my husband felt the brunt of my stress. Something had to give, but I didn't want my commitments to lessen. So I invested in one-one sessions in transcendental meditation (TM). I didn't buy into the whole TM lifestyle, I only took what in needed from it. My life started to feel more balanced. I became calmer, more relaxed but at the same time my clarity of thought improved. My husband noticed the difference within 2 months, my son commented 'Mummy, you are nicer and fun when you have done quiet time'. Over the years, as with any new technique we learn, keeping the momentum started to falter. Then I read about Andy Puddicombe and his App for mindfulness meditation. I thought, why not give it a try? It is one the best decisions I made last year. My sense of calm and focus has increased. I perform well in pressurised situations. My anaesthetist attached me to monitoring devices, and my heart rate & blood pressure is lower. TM was a calming type of meditation technique, whereas this app has taught me a combination of both insight and calm. Go get it! Give it a try! Watch this little animation by clicking on the link below: http://www.getsomeheadspace.com/News/headspace-extra/the-headspace-animations--expectation.aspx (I have no conflicts of interest to declare).  I was invited by the BAPRAS President to an interesting event last week at RBS Bishopsgate, London- 'Inspiring Women Leaders' a book launch by Lee Travers, an executive coach who has distilled the qualities that successful leaders possess. When it comes to surgical training, as a plastic surgery trainer, I am seeing more women choosing this career path, especially as the intake in medical schools is 60% female. For my generation, the gender of the trainee surgeon is irrelevant. What is crucial is surgical ability, insight and empathy for patients. There is also this nebulous elephant in the room: the confidence - competence gap. The dissociation between these two elements is most noticeable at the ends of the spectrum. On one hand, there are trainees who over-estimate their ability to perform a surgical task. Their profiles and attitudes to risk are perhaps similar to those encountered in other industries such as investment / banking sectors. At the other end of the spectrum, there are those who need mentoring and nurturing to encourage self-belief. Many, however, are in the middle of the spectrum: have insight, and know their limits. As a trainer, I have to identify where the trainee is on this spectrum, and help him/her to explore their potential to its maximum. They are the future of our profession. I remember the day, 25 years ago, a naive 19 year old telling my father, a general surgeon & fellow of The Royal College of Surgeons of England (RCSE), that I wanted to pursue a career in surgery. He advised me against it as it would be too difficult, not suited for women and suggested a non-surgical speciality. His words were not dissimilar to those of Prof Meirion Thomas in his article in the Daily Mail. The difference is that my father, now 78, has changed his views and moved with the times. Especially as I have made him proud on three occasions: the first, when I passed each of my FRCS exams at the first attempt; the second, when I received the Hunterian Professorship by the RCSE in 1999-2000; the third, when I was appointed as the first female consultant plastic surgeon at the world-famous Queen Victoria Hospital, East Grinstead- the home of Archibald Mcindoe & the guinea-pigs, and where the first Microvascular Toe-Thumb transfer by John Cobbett was carried out in 1969.
In my career so far, I have not been subject to any overt sexism or racism. If there has been anything covert, my in-built mechanism of being blind & deaf to it has certainly made me immune, as such issues are not of my making but is the burden that the perpetuator carries. As a woman, I have had to work harder, be supremely organised in both my work and home life, be diplomatic but hold my ground, just so I could be on par with my male peers in my early career. Now, with more women choosing a career in surgical specialities; colleagues of my generation feel that the gender of the surgeon is irrelevant, more important is surgical ability and insight. The response from the RCSE President has been heartening. Striving for a work-life balance is not just something women want, as I do too; but so does each of my male colleagues of my generation where I work: we all want time to have a life outside of work, see our children grow up, rather than Daddy (or Mummy) be a sticker on the fridge. Life-work balance makes us well-rounded contributors to society, helps us to empathise with our patients and involve them in their care, rather than have the paternalistic & patronising personas of surgeons of my father's generation. Ours is a different generation, with different needs in an NHS that has undergone a radical culture change. Attitudes such as those Prof Meirion Thomas that breed intolerance of women in surgical specialities, should stay where they belong, in the last century. I wholly concur with the view held by the Chief Executive of NHS Employers "Some people are women, get over it." |
Archives
February 2020
Categories
All
|




 RSS Feed
RSS Feed





